Spring is here. The trails are calling. Your team’s season is underway. And you’re still on the sidelines, wondering when — or if — it’s okay to get back out there.
If you’ve been living with a concussion or post-concussion symptoms, that question probably feels equal parts hopeful and terrifying. You want your life back. But you’ve also felt what happens when you push too hard, too soon.
Returning to exercise after a concussion isn’t a guessing game — but it’s not a simple checklist either. The process is deeply individual, and what helps one person at six weeks post-injury could set another person back significantly. If you’ve been getting vague answers, that’s not an accident. This is genuinely one of the more nuanced parts of recovery. Here’s an honest look at what it actually involves.
Why Exercise Matters More Than You Might Think
For years, the standard advice after a concussion was simple: rest. Stay in a dark room. Avoid screens. Don’t do anything that makes your symptoms worse.
We now know that strict, prolonged rest can actually slow down recovery.
Your brain relies on something called neurovascular coupling — the synchronized relationship between blood flow and neural activity. When that relationship gets disrupted by a concussion, the brain struggles to regulate itself during physical or cognitive effort. The result: brain fog, fatigue, headaches, and that overwhelming sense of crashing after even a small amount of exertion.
But here’s the key: gentle, controlled exercise is one of the primary ways to retrain that system. It prompts neuroplasticity, regulates blood flow, and helps the brain learn to handle demand again — carefully, incrementally, and with the right support.
The goal isn’t to avoid activity forever. It’s to reintroduce it at the right pace.
The Problem with Returning Too Soon
Most people who’ve dealt with a concussion know this feeling: you have a few good days, start to feel like yourself again, and decide you’re ready to jump back in. You go for a run. You hit the gym. You push through a workout.
And then you pay for it.
This is called a symptom flare cycle, and it’s one of the most common — and frustrating — parts of concussion recovery. When you push your brain past its current capacity, symptoms return (sometimes worse than before), and your recovery can actually regress.
Returning to exercise too early isn’t just uncomfortable. It can extend your timeline by weeks or even months.
This is why the question isn’t just “can I exercise?” — it’s “is my brain ready for this specific level of demand?”
5 Signs You May Not Be Ready Yet
Before jumping back into exercise, honestly check in with yourself on these:
You’re relying on willpower to push through. Determination is admirable. But in concussion recovery, pushing through symptoms doesn’t build resilience — it delays it. Seek support to stop those workaround patterns and start genuinely healing.
You’re still symptomatic at rest. If you have regular headaches, brain fog, or dizziness even when you’re not doing anything demanding, your baseline isn’t stable enough for exercise to help.
Light activity causes a symptom spike. A short walk, light household tasks, or even a casual conversation that makes your symptoms worse is a signal your nervous system is still in a fragile state.
Your symptoms take a long time to recover after exertion. Feeling worse after activity for a few hours is one thing. Feeling worse for days is another. The longer the recovery window, the more cautious your approach needs to be.
You haven’t been cleared by a professional. A general “you’re good to go” from someone who hasn’t specifically assessed your neurovascular function is not the same as a targeted clearance. Make sure someone who understands brain injury has evaluated where you actually are.
What a Graduated Return-to-Activity Protocol Actually Looks Like
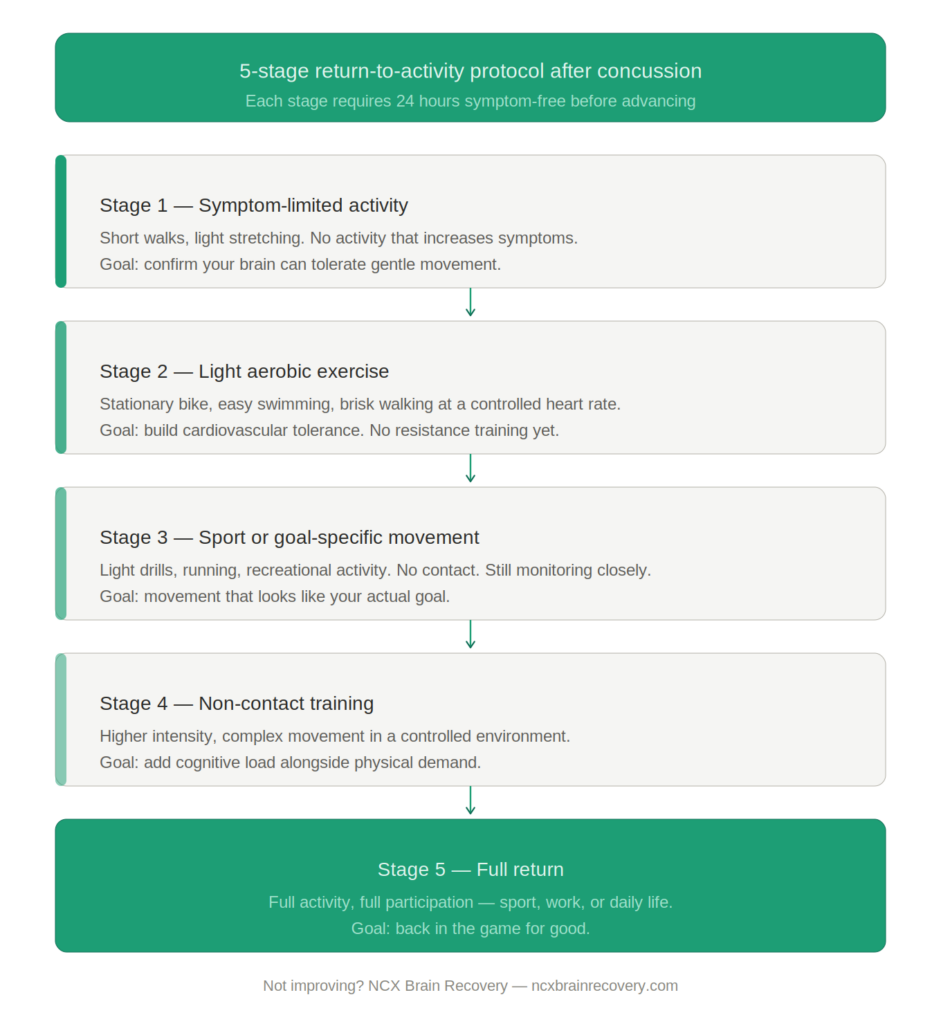
Why Many People Get Stuck — And What Actually Helps
We see it regularly: someone comes in after weeks — sometimes months — of doing everything they were told. Resting. Avoiding screens. Waiting it out. And they’re not better. In some cases, they’re worse. They’ve been patient, they’ve followed the rules, and still nothing has changed. That’s not a personal failure. It’s a sign that rest alone was never going to be enough.
Here’s why: rest can reduce acute inflammation and give the brain a chance to stabilize — and that matters, especially early on. But it doesn’t rehabilitate the underlying dysfunction. If your brain’s visual system, vestibular system, autonomic regulation, and neurovascular coupling are still disrupted, time and stillness won’t fix them. The brain will simply keep compensating — working around the problem rather than through it.
If you’ve been resting for weeks or months with no real improvement, that’s often a sign you’ve moved past what rest can do. It’s time for a different approach.
At NCX Brain Recovery, our multi-sensory approach works on the whole brain — not just managing symptoms, but addressing the compensation patterns that keep people stuck. By engaging vision, vestibular function, autonomic regulation, and neurovascular coupling together, we give the brain what it needs to stop working around its dysfunction and actually heal. When that happens, the return to activity becomes sustainable in a way that rest alone never achieves.
Our patients don’t just get cleared to exercise. They come back to sport, work, and life with a brain that’s actually prepared for what’s ahead.
You Don’t Have to Keep Guessing
If you’re months into recovery and still not sure where you stand — still holding back because you’re afraid of a setback — that uncertainty doesn’t have to be permanent.
A targeted assessment can tell you exactly where your brain is in the recovery process, what’s still limiting you, and what a realistic return-to-activity plan looks like for you specifically.
Not sure where you’re at in recovery? Schedule a free consultation with our team. We’ll help you figure out where you are — and what it actually takes to get you back in the game.
